Facing Brain Tumors: Is Surgery Still the Best Option?
Facing Brain Tumors: Is Surgery Still the Best Option?
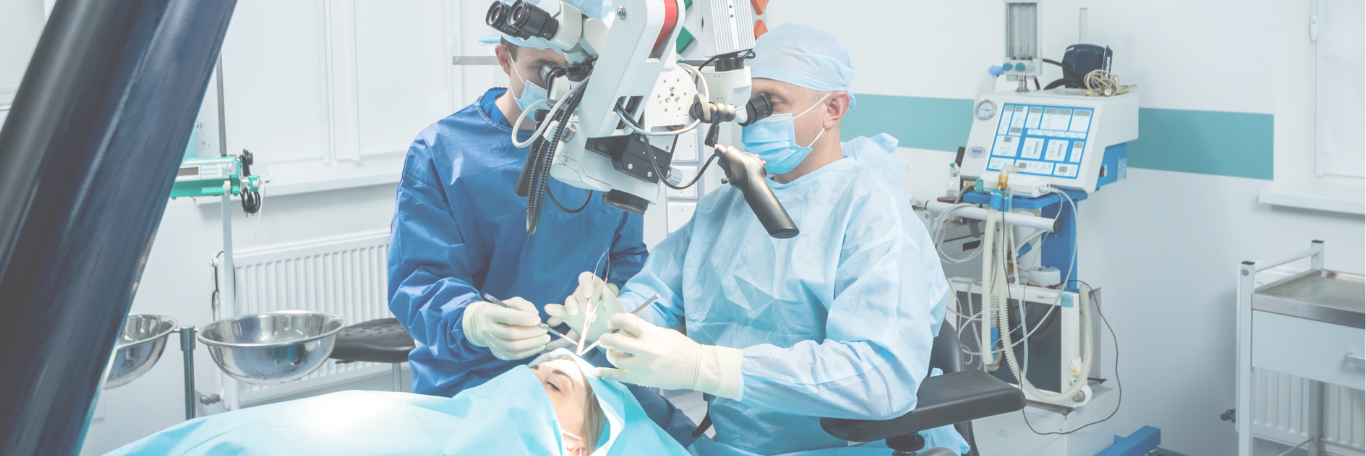
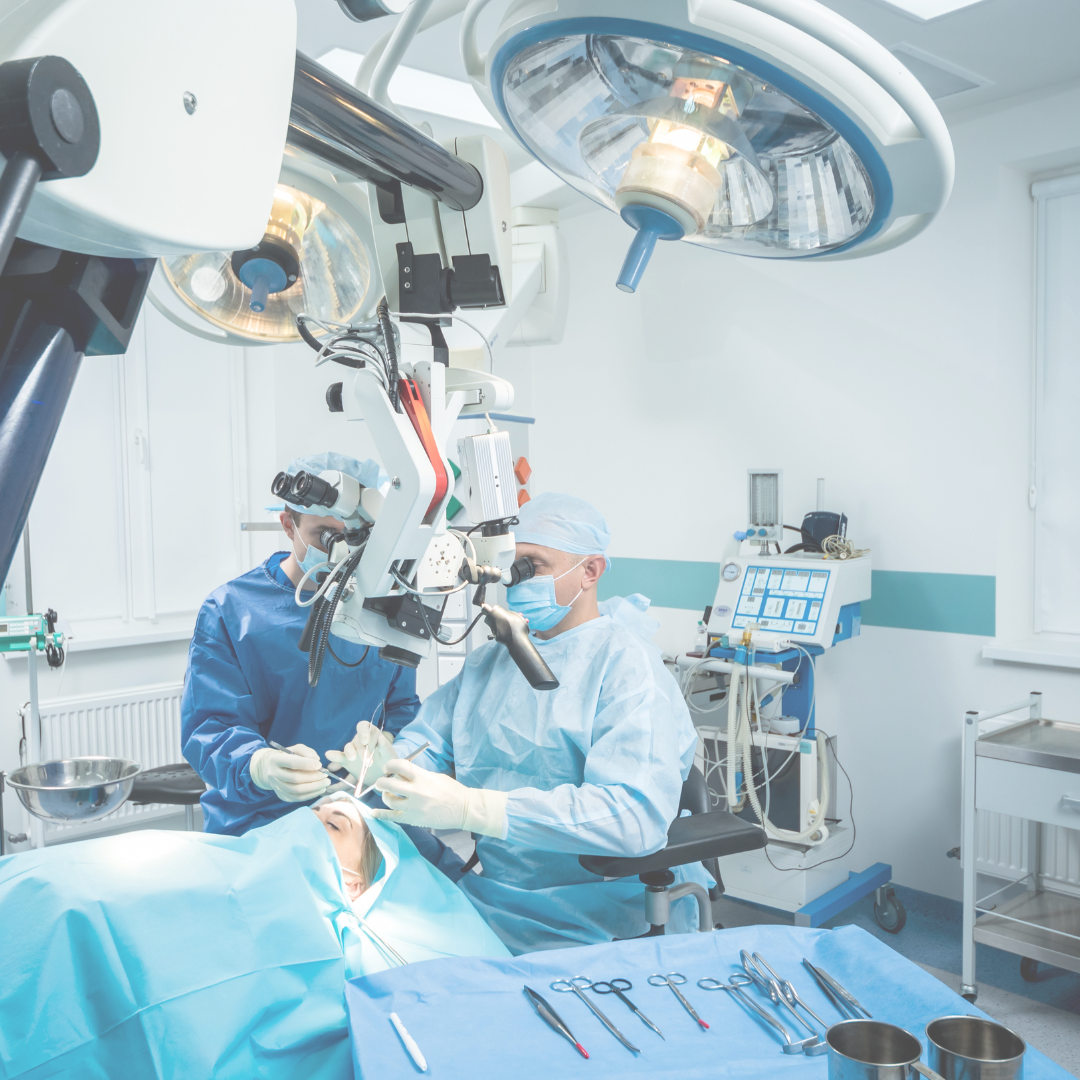
For many brain tumor patients, surgery is the preferred treatment option as it allows for the removal of tumor tissue.
Glioblastoma multiforme (GBM) is one of the most common and aggressive types of brain tumors, typically occurring in adults and older individuals. Due to its rapid growth and resistance of brain cancer cells to chemotherapy, treatment becomes highly challenging. Additionally, a high proportion of cancer stem cells make brain tumors prone to recurrence and difficult to treat, resulting in an average survival period of only 4 to 6 months after recurrence. For many brain tumor patients, surgery is the preferred treatment option as it allows for the removal of tumor tissue. However, to preserve surrounding vital neural structures, surgery typically employs the maximal safe resection approach. Since the human brain cannot sacrifice peripheral tissues like tumors in other parts of the body, residual cancer cells may remain after surgery. To improve treatment outcomes, adjuvant therapies such as radiation therapy, chemotherapy, or targeted therapy are often combined postoperatively.
Current Brain Tumor Treatment Options
According to statistics from the American Cancer Society (ACS) and the Central Brain Tumor Registry of the United States (CBTRUS), an estimated 20,000 new cases of brain tumors are diagnosed each year, with approximately 400 new cases of malignant gliomas reported annually in Taiwan.

Gold Standard Therapies
- Surgery: For most brain tumor patients, surgery is the primary and most common treatment method. Common surgical procedures for brain tumors include craniotomy, MRI-guided laser ablation, endoscopic brain tumor surgery, and neurosurgical tubular retractor systems. However, surgery may not be feasible for tumors with unclear boundaries, those located close to vital brain regions governing vision, language, or motor functions, or cases where surgery risks significant functional impairment postoperatively.
- Radiation Therapy: Often administered after surgery, radiation therapy targets residual cancer cells that cannot be completely removed during surgery. It involves using high-energy gamma rays or other radiation to destroy GBM tumor cells. External beam radiation therapy delivers radiation from an external machine directed at specific areas of the patient’s body to kill tumor cells. Radiation therapy is commonly used as an adjunctive treatment following surgery and may cause side effects such as fatigue, nausea, vomiting, headaches, and skin rash.
- Chemotherapy: The current frontline chemotherapy drug is TEMODAL, which exhibits antitumor activity and contains an alkylating agent with an imidazotetrazine ring. Administered orally in combination with radiation therapy, chemotherapy is continued until patient conditions improve, with treatment durations ranging from 6 to 12 months, up to a maximum of 2 years. Side effects may include nausea, vomiting, and others. Clinical trial data show a median survival of 5.8 months for recurrent patients treated with TEMODAL. However, oral medications are often limited by the blood-brain barrier, resulting in limited drug delivery to the tumor site and systemic side effects that may negatively impact patients’ quality of life.
Other Treatment Methods
- Targeted Chemotherapy: Monoclonal antibody bevacizumab is commonly used for the treatment of brain tumors, including GBM. Its mechanism of action involves inhibiting tumor angiogenesis to slow or stop tumor growth.
- Tumor Treating Fields (TTFields) Therapy: TTFields therapy is a relatively new treatment modality that utilizes a portable device to deliver alternating electric fields at specific frequencies, selectively targeting and killing tumor cells through various mechanisms. Approved by the Taiwan Ministry of Health and Welfare in May 2023, this therapy is currently not covered by national health insurance and is considered a self-pay option.
- Clinical Trials: Participation in clinical trials (referring to our company’s new drug development project) provides patients with access to the latest treatment methods and medical technologies, thereby improving treatment efficacy and quality of life.
Maximal Safe Resection
The primary treatment modality for GBM is surgery, aiming for maximal safe resection of the tumor without causing damage to surrounding healthy brain tissue. However, GBM tumor cells typically infiltrate surrounding tissues, making complete tumor resection impossible. Therefore, numerous studies have highlighted the correlation between overall survival and the extent of resection. In this context, adjunctive techniques during neurosurgical procedures to expand the resection boundaries or precisely delineate tumor margins have become crucial factors.
More Precise Tumor Resection
- Fluorescence-Guided Surgery: 5-Aminolevulinic Acid (5-ALA) is an adjuvant agent used in resection surgery for malignant brain tumors. Patients ingest 5-ALA 2-4 hours before surgery, which is then absorbed by tumor cells and converted into PPIX. During surgery, tumor cells exhibit red fluorescence when excited by blue light. Fluorescence-guided surgery, combined with intraoperative microscopic neurofunctional monitoring, helps surgeons enhance tumor cell clearance and improve patient survival rates.
- Awake Brain Tumor Surgery: This procedure is performed with the patient awake but sedated, allowing neurosurgeons to stimulate specific brain regions during surgery to identify crucial functional areas to avoid. Awake brain tumor surgery is typically employed for tumors that are difficult to remove conventionally due to size or location, or those with indistinct boundaries and extensive brain involvement. During the procedure, neurosurgeons use small electrodes to stimulate areas surrounding the tumor, and patients are asked to perform various tasks to ensure the preservation of vital brain functions. Neurosurgeons create maps of brain functional areas using preoperative and intraoperative brain imaging and patient responses. They then attempt to remove the tumor as extensively as possible while avoiding functional brain regions. Throughout the surgery, a neuroanesthesiologist ensures that patients do not experience any pain, monitors vital signs, and engages in conversation to help them remain calm.
- Intraoperative MRI and Second Stage Resection: During brain cancer surgery, the soft and easily displaceable nature of brain tissue can complicate preoperative localization and reduce resection accuracy, often necessitating repeated craniotomies for patients. Utilizing an MRI system intraoperatively allows surgeons to re-localize and visualize real-time changes in the brain as well as the position and size of any remaining tumor. This can help avoid excessive or insufficient tumor removal. For example, at National Taiwan University Hospital, over 70% of patients who undergo re-localization with intraoperative MRI require a second stage resection.
- FastGlioma (clinical stage): Utilizing a large amount of unlabeled optical microscopic imaging AI self-learning technology, clinical trials have confirmed that it significantly outperforms traditional image-guided and fluorescence-guided auxiliary methods in detecting tumor infiltration during surgery. In rapid mode, this technology requires only 10 seconds to obtain a low-resolution image, while still achieving a recognition accuracy of up to 92%. We hope this technology can be quickly applied in clinical settings to assist surgeons in determining whether a second surgery is needed to remove residual cancer cells. (Source: nature)

Glioblastoma Patients Aged 70+: Active Treatment is Key to Prolonging Survival
A recent study published in Cancers (tracking through 2025, involving 124 patients aged ≥70 with a median overall survival [mOS] of ~8 months) indicates that glioblastoma patients over the age of 70 should not forgo treatment solely due to their age. The research demonstrates that active, multimodal treatment regimens can still provide significant survival benefits for elderly patients.
Two Core Factors Influencing Survival:
Extent of Surgical Resection: Patients achieving “Gross Total Resection” (GTR) show a significantly better prognosis compared to those with only partial resection.
Adjuvant Therapy: Post-operative combination of radiotherapy and chemotherapy effectively extends life, with the most pronounced benefits observed during early intervention.
The study also found that chronological age and pre-operative health status were not the key determinants of survival; however, a history of smoking was significantly associated with poorer outcomes.
Cerebraca® Wafer: Optimizing Postoperative Prognosis for GBM
A key focus of Cerebraca® Wafer is to eradicate residual tumor cells and suppress cancer stem cells after brain surgery. Implanted at the surgical resection site, Cerebraca® Wafer creates a localized high-concentration drug environment with good penetration and sustained drug release for up to 30 days, inhibiting the growth of residual tumor cells.
Post-Surgery Care for Brain Tumor Patients
Postoperative care
Postoperative care following brain tumor surgery is crucial to the patient’s prognosis. Key care measures include closely monitoring the surgical wound for abnormal fluid leakage or bleeding, managing the drainage tube, and effectively controlling pain. Additionally, it’s important to prevent symptoms like vomiting or seizures. If the patient is unable to move independently, they should be assisted with regular repositioning to avoid pressure sores. Attention to diet is also critical to prevent aspiration pneumonia. Finally, patients should avoid straining or exerting pressure, as this can elevate intracranial pressure and hinder wound healing.

Listening to music can help patients reduce pain and improve recovery outcomes
At the 2024 American College of Surgeons (ACS) Annual Meeting, researchers presented a study about how music can help reduce the need for pain medications in post-surgery patients. The study found that listening to music during recovery can effectively reduce anxiety, pain, and stabilize heart rates. Patients who received music therapy required only half the amount of morphine compared to those who did not listen to music.
The study emphasized that music can aid in reducing stress as patients recover from surgery. Researchers noted that music could lower cortisol (the stress hormone) levels, which may help decrease the perception of pain. Patients are encouraged to listen to familiar and comforting music, as it enhances the soothing effect and potentially speeds up recovery. (original source)

Balanced Diet
A well-balanced diet can assist in body restoration and improve physical strength. It is advisable to consume fresh vegetables and fruits while reducing the intake of high-fat, high-sugar, and processed foods. It is essential to follow the physician’s advice for a balanced diet.
read more👉Balanced Diet for Cancer Patients
Reference
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/brain-tumor/brain-tumor-treatment
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/brain-tumor/brain-tumor-surgery
- https://www.mdpi.com/2076-3425/13/2/216
- https://link.springer.com/article/10.1007/s11060-020-03494-9
- https://www.jstage.jst.go.jp/article/nmc/52/8/52_3136/_article
- https://udn.com/news/story/7266/7332857
- https://www.ntuh.gov.tw/BMED/Fpage.action?muid=3901&fid=3683
- https://udn.com/news/story/7266/8143080
- https://fastglioma.mlins.org/